Adverse Hemodynamic Effects of Nefopam in Patients Undergoing Plastic and Aesthetic Surgery: A Single-Center Retrospective Study
Article information
Abstract
Background
Nefopam is used to improve postoperative hypothermia in the field of plastic and aesthetic surgery. However, there is a paucity of data about its adverse hemodynamic effects and safety. We therefore assessed its adverse hemodynamic effects in patients undergoing plastic and aesthetic surgery.
Methods
We conducted a single-center retrospective study of 148 patients, in whom we measured hemodynamic parameters using sphygmomanometry (systolic blood pressure [SBP], diastolic blood pressure [DBP], arterial blood pressure [ABP], and heart rate [HR]). Moreover, we also assessed myocardial oxygen demand using the rate pressure product (RPP).
Results
The patients included 96 men and 52 women, with a mean age of 34.7±8.5 years. There were no significant differences in SBP, DBP, ABP, HR, or RPP before and after nefopam administration (P>0.05). However, a significant difference was found in the number of the patients with an HR of >100 beats per minute or with an RPP of >12 U before and after nefopam administration (P=0.001).
Conclusions
Surgeons should consider the possibility of tachycardia and increased blood pressure in the management of postoperative hypothermia in patients with cardiac arrhythmia, ischemic heart disease, or essential hypertension. Nonetheless, further prospective, large-scale, multi-center, randomized, controlled studies are warranted to confirm our results.
INTRODUCTION
Multimodal analgesia is the most widely used strategy for treating patients with acute postoperative pain [1,2]. Postoperatively, it has a higher degree of analgesic effect and safety than unimodal analgesia [3]. Postoperative pain relief is a key issue that is closely associated with patient care and satisfaction, making it an important component of postoperative outcomes. Non-steroidal anti-inflammatory drugs (NSAIDs) and opioids are typically used for postoperative pain relief.
Nefopam is a non-opioid analgesic that is used to improve postoperative pain [4], and it is generally known to be safe and well-tolerated. Most of the reported adverse effects include drowsiness, nausea and vomiting, and sweating [5]. In addition, its potentially more serious adverse effects include confusion and tachycardia. Unlike NSAIDs, it has no effect on platelet function, and unlike opioids, it does not raise the risk of respiratory depression [6,7].
There is a growing interest in postoperative hypothermia in surgical settings because it may lead to postoperative complications, a slower recovery, and poor outcomes [8]. Thus, it is considered a patient safety concern, and has been investigated in an increased number of published studies over the past decade. To date, efforts have been made to identify its impact on patients undergoing surgery and the optimal treatment strategies for such patients. Moreover, studies have investigated methods for preventing the occurrence of postoperative hypothermia and thereby minimizing its detrimental effects. According to a literature review, approximately 50% to 90% of patients who undergo surgery are vulnerable to postoperative hypothermia in the absence of active warming strategies [9,10]. Diverse modalities are effective for preventing and treating postanesthetic shivering, including α2 agonists, tramadol, meperidine, and serotonin-3 receptor antagonists [11-17]. However, there is still no gold standard in this context. Nefopam is a promising drug because it is effective, but does not cause serious adverse effects [18-21]. In addition, it is also used to improve postoperative hypothermia in the field of plastic and aesthetic surgery. To our knowledge, however, there is a paucity of data about its adverse hemodynamic effects and safety.
Given the above background considerations, we conducted this study to assess the adverse hemodynamic effects of nefopam in patients undergoing plastic and aesthetic surgery.
METHODS
This single-center retrospective study was approved by the Institutional Review Board of our medical institution. Informed consent was waived due to its retrospective nature. We enrolled a total of 148 patients who had undergone plastic surgery at our institution between August 2014 and February 2017. Informed consent was waived due to the retrospective nature of this study.
We included patients who received nefopam after plastic and aesthetic surgery, with an American Society of Anesthesiologists physical status of class I and II, and without an allergic or hypersensitivity reaction to nefopam. However, we excluded patients aged ≤18 years or ≥60 years, those with tachycardia (defined as a heart rate [HR] ≥100 beats per minute [bpm]), atrial fibrillation, arterial hypertension, anemia, hypothyroidism, or epilepsy, as well as those who were deemed to be ineligible for study enrollment according to our judgment.
Anesthetic protocol
Anesthetic management was provided by balanced general anesthesia with mechanical ventilation. Anesthesia was induced via the intravenous administration of a bolus of fentanyl (50–100 μg), thiopental sodium (3–6 mg/kg) and rocuronium bromide (0.8 mg/kg) with a subsequent bolus or microfluidic administration of a muscle relaxant. Anesthesia was maintained via inhalation of sevoflurane (minimum alveolar concentration [MAC] of 0.6–1.0%) and the bolus or microfluidic administration of fentanyl (0.05 mg/h). Ketorolac tromethamine (30 mg) was intravenously administered for 20 to 30 minutes before the end of surgery to achieve preemptive anesthesia. All patients received dexamethasone (4 mg) before the start of surgery. Nefopam hydrochloride (Acupan®; Pharmbio Korea, Chungju, Korea) was intramuscularly administered once shortly after surgery (1.9±1.2 hours) at a dose of 20 mg.
Patient evaluation and criteria
To assess the effects of nefopam on the hemodynamic profile in our clinical series of patients, we performed a retrospective analysis of their medical records and evaluated their baseline and hemodynamic characteristics.
The baseline characteristics included age, sex (male or female), and the type of surgical procedure. In addition, the hemodynamic characteristics included systolic blood pressure (SBP), diastolic blood pressure (DBP), arterial blood pressure (ABP), and HR.
The rate pressure product (RPP) was used to assess myocardial oxygen demand, and was calculated using the following formula [22]:
RPP (U)=(SBP×HR)÷1000
The hemodynamic profile of the patients was compared before and after nefopam administration. We then calculated the number and percentage of the patients with an HR >100 bpm or an RPP of >12 U.
For safety assessment, we examined whether our clinical series of patients presented with treatment-emergent adverse events (TEAEs) and then compared their frequencies before and after nefopam administration.
Statistical analysis
Statistical data analysis was performed using Microsoft Excel 2010 (Microsoft Corp., Redmond, WA, USA) and Statistica 6.0 (StatSoft Inc., Tulsa, OK, USA). All data were expressed as mean±standard deviation. Differences in hemodynamic characteristics before and after nefopam administration were analyzed using the Student t-test. All P-values of less than 0.05 were considered to indicate statistical significance.
RESULTS
Baseline characteristics of the patients
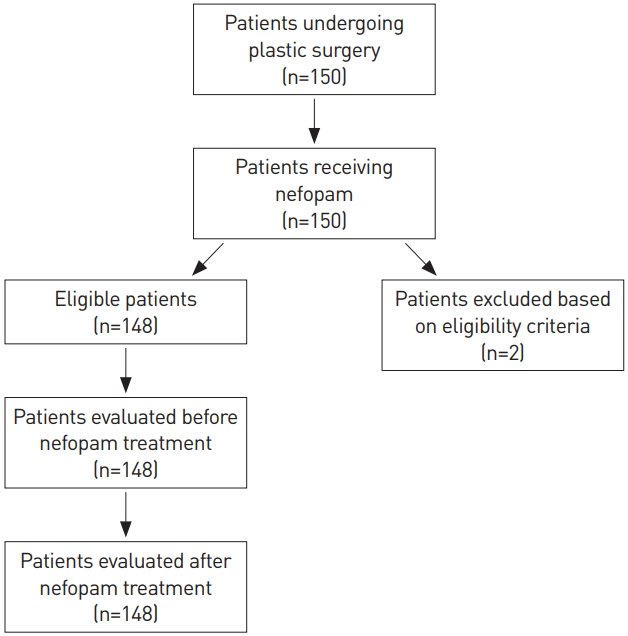
A total of 148 patients were evaluated in the current study (Fig. 1). Our clinical series of patients included 96 men and 52 women, with a mean age of 34.7±8.5 years. The number of patients undergoing breast surgery, scar revision, rhinoplasty, osmidrosis surgery, liposuction, and dacryocystorhinostomy was 71 (48.0%), 31 (20.9%), 17 (11.5%), 14 (9.5%), 11 (7.4%), and 4 (2.7%), respectively. Their baseline characteristics are summarized in Table 1.
Hemodynamic changes after nefopam administration
In our series, increases in SBP, DBP, ABP, HR, and RPP were found after nefopam administration, but these differences did not reach statistical significance (Table 2). No patients had an HR of >100 bpm before nefopam administration, while 26 (17.6%) did so after nefopam administration. This difference reached statistical significance (P=0.001). In addition, 3 patients (2.0%) had an RPP of >12 U before nefopam administration, whereas 8 (5.4%) did so after nefopam administration. This difference was also statistically significant (P=0.001).
DISCUSSION
Postoperative pain may cause postoperative complications, such as atelectasis, hypertension, delirium, a prolonged hospital stay, and a lower level of patient satisfaction with the postoperative outcomes. Patient-controlled analgesia (PCA) is known to reduce the intensity of postoperative pain and complications more efficiently than conventional types of opioid analgesia. NSAIDs have been used in combination with opioids (such as fentanyl, morphine, or oxycodone) for PCA, since they were first found to reduce opioid consumption and opioid-related adverse effects. However, they may affect platelet function, potentially leading to an increased bleeding tendency and adverse gastrointestinal effects. It has been reported that bolus administration of nefopam (every 4 hours for 24 hours) showed a significant morphine-sparing effect without causing clinically noteworthy adverse effects [23].
A 30% to 40% decrease in the use of opioids has been documented when nefopam was postoperatively administered [24,25]. Additionally, another report found that its use resulted in decreased morphine consumption when it was used for multimodal analgesia in surgical settings [26]. The mechanisms underlying its anti-shivering effects and thermoregulatory actions are not completely understood. It is presumed, however, that it inhibits the synaptic reuptake of dopamine, norepinephrine, and serotonin, as amphetamine does. Moreover, it has been suggested to be involved in the thermoregulatory response via α2 adrenoceptors [27,28].
The use of infiltration anesthesia in the field of plastic surgery has become popular, leading to favorable conditions for multimodal analgesia in the early postoperative period [22]. Considering the low trauma rate of most plastic and aesthetic surgical procedures, non-opioid drugs play a key role in postoperative pain relief [29]. Because non-opioid analgesics do not cause residual sedation or cognitive impairment, patients can be active in the first postoperative hours, thereby preventing thrombotic and thromboembolic complications [30,31]. NSAID use for postoperative pain relief has some restrictions, due to the risk of gastroduodenal damage and renal papillary necrosis with subsequent renal failure in patients with concomitant gastric and renal pathologies [32,33]. However, these complications should be considered as potential risks when prescribing NSAIDs in aesthetic medicine. In aesthetic surgery, more attention is devoted to potential bleeding disorders resulting from platelet dysfunction when using high doses of NSAIDs, and to the possibility of diffuse bleeding in the integumentary area after aesthetic and plastic surgery [34,35]. Nefopam has no effect on platelet function, yet provides comparable pain relief to NSAIDs [36-38]. In addition, nefopam can be used in combination with NSAIDs and opioid analgesics. Because they have different mechanisms of analgesia, drug combinations can be used safely and effectively [39,40]. In contrast with nefopam, which has a central mechanism of action, NSAIDs have a peripheral action at the site of the damaged tissues [41]. A powerful, synergistic analgesic effect has been reported from the concomitant use of nefopam and ketoprofen, with a significantly reduced drug dose required for full pain relief. After abdominal and orthopedic surgery, nefopam exhibited a morphine-sparing effect, with 30% to 50% decreased morphine demand during PCA [5].
Previous studies have performed detailed analyses of the side effects associated with nefopam. Minor side effects in the form of nausea, vomiting, dizziness, increased perspiration, erythema, and anxiety were reported in 15% to 30% of patients using nefopam [42]; rare cases of overdoses of the oral drug form with seizures and arrhythmia have also been reported [43,44]. Our data do not confirm a high frequency of minor side effects associated with nefopam, which is explained by the use of balanced general anesthesia and by the use of dexamethasone to prevent postoperative nausea and vomiting. Tachycardia and increased blood pressure after intramuscular drug administration are particularly noteworthy, both of which are associated with the anticholinergic and sympathomimetic properties of a drug [45]. However, this effect has not been demonstrated in the literature for nefopam. In our study, 26 (17.6%) and 8 (5.4%) patients had an HR of >100 bpm and an RPP >12 U, respectively, after nefopam administration. A similar hemodynamic effect was observed in early clinical trials after the intravenous administration of a bolus of nefopam; this negative effect decreased after transitioning to a slow drug infusion over 30 minutes [42]. Changes in the circulatory response should be considered in the postoperative period in patients with ischemic heart disease and arrhythmia. Additionally, it should be noted that hypertension is undesirable after face lifts due to the risk of hematomas in the surgical area [46]. It can therefore be inferred that nefopam should not be administered to patients with essential hypertension undergoing plastic and aesthetic surgery.
In our series, there were some cases of TEAEs. To date, however, few studies have examined TEAEs associated with nefopam [47,48]. In 1980, sweating, nausea and sedation were first described as the most frequent TEAEs [47]. Moreover, the safety profile of nefopam was reported during a 12-year period ranging from 1982 to 1994 and then analyzed [48]. Since 1995, however, no accurate data have been published about this issue. Nonetheless, surgeons should consider the possibility of TEAEs associated with nefopam when using it in the postoperative period.
To summarize, our results showed not only that there were no significant differences in SBP, DBP, MBP, HR, or RPP before and after nefopam administration, but also that there were significant differences in the number of patients with an HR of >100 bpm or an RPP of >12 U before and after nefopam administration (P>0.05 and P=0.001, respectively).
Nonetheless, our results cannot be generalized, not only because we analyzed a small number of patients using a retrospective design, but also because we did not evaluate patients who received a repeated or continuous infusion of nefopam over several days, analyze the causal relationship between TEAEs and nefopam, or compare nefopam infusion with other analgesics.
In conclusion, our results indicate that surgeons should consider the possibility of tachycardia and increased blood pressure in the management of postoperative hypothermia in patients with cardiac arrhythmia, ischemic heart disease, or essential hypertension. Further prospective, large-scale, multi-center, randomized, controlled studies are warranted to confirm our results.
Notes
No potential conflict of interest relevant to this article was reported.