INTRODUCTION
Breast augmentation surgery has been the most popular cosmetic surgery in the United States since 2006, accounting for 290,000 cases in 2013 [1]. Unfortunately, complications from the procedure can result in a reoperation rate approaching 15.5%. Complications after breast augmentation include capsular contracture, size change, malposition, waviness, deflation, infection, ruptured gel, palpability, and anxiety [2].
ŌĆśBottoming outŌĆÖ is the term that describes an increase of the distance between the nipple areolar complex and the inframammary fold. In augmented breasts, inferior displacement of the breast implant beyond the inframammary fold can also be a causative factor. There are numerous procedures for correcting bottoming out, such as single or multilayer capsulorrhaphy, with or without mirror-image selective capsulotomy [3,4], capsulopexy [5], capsular flaps [6], polypropylene mesh, cadaveric dermis, and intracapsular allogenic dermal grafts [7-9]. However, these methods have drawbacks of larger incisions, longer surgical time, and possibility of infection caused by allogenic materials. Longer surgical time and costly allogenic materials can be sources of complaints and a burden for both the surgeon and the patient. In this case report, we propose a simple procedure for correcting an inferiorly malpositioned implant via an endoscopic approach.
CASE REPORTS
Case 1
A 29-year-old woman who underwent transumbilical breast augmentation with an Allergan (Allergan, Inc., Irvine, CA) style 410 MF anatomically textured, form stable, 295-g implant came to our outpatient clinic, presenting with inferior displacement of the breast implant. Her condition was corrected using our novel method with a Bovie electrocoagulator using an endoscopic approach.
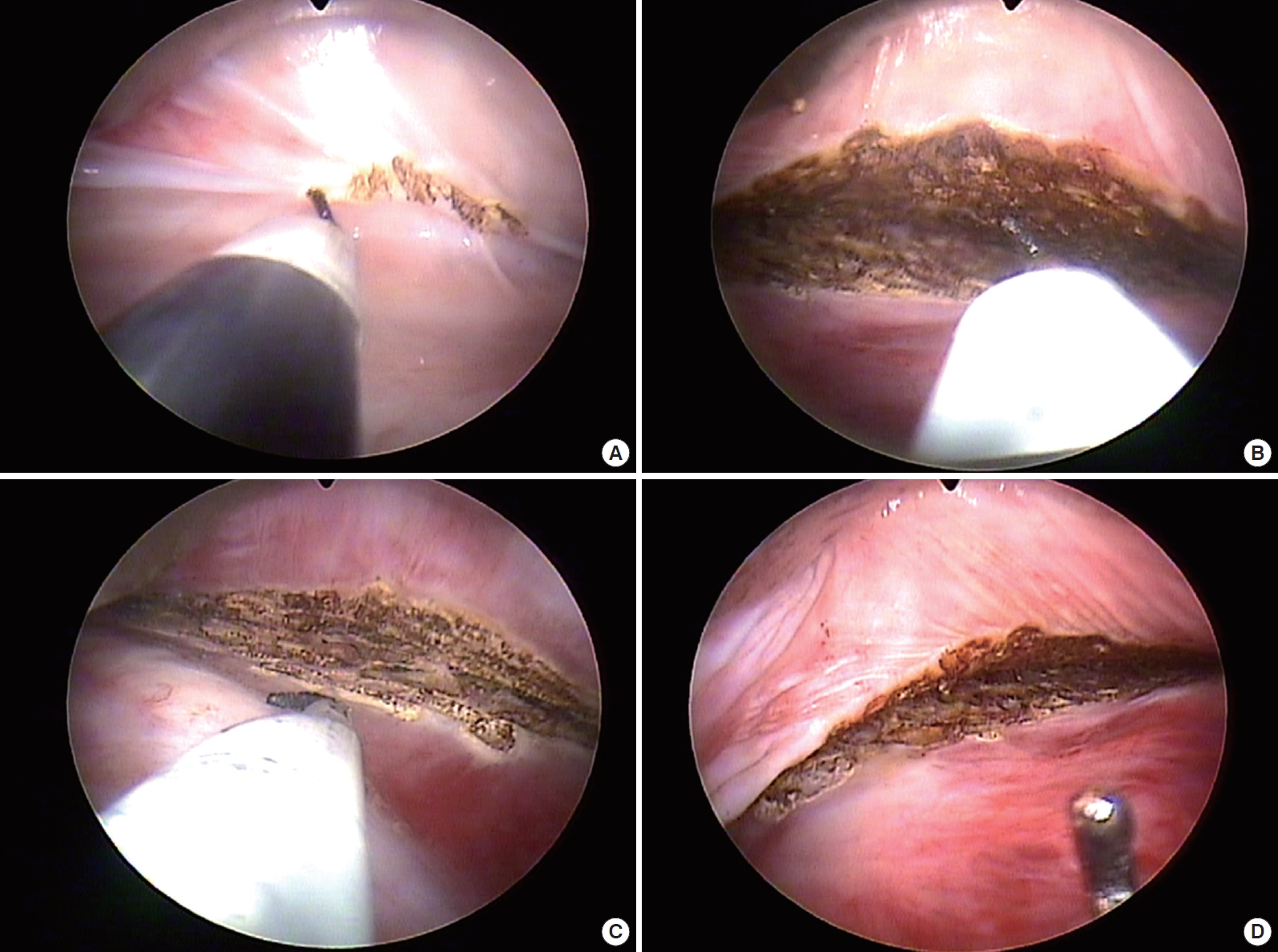
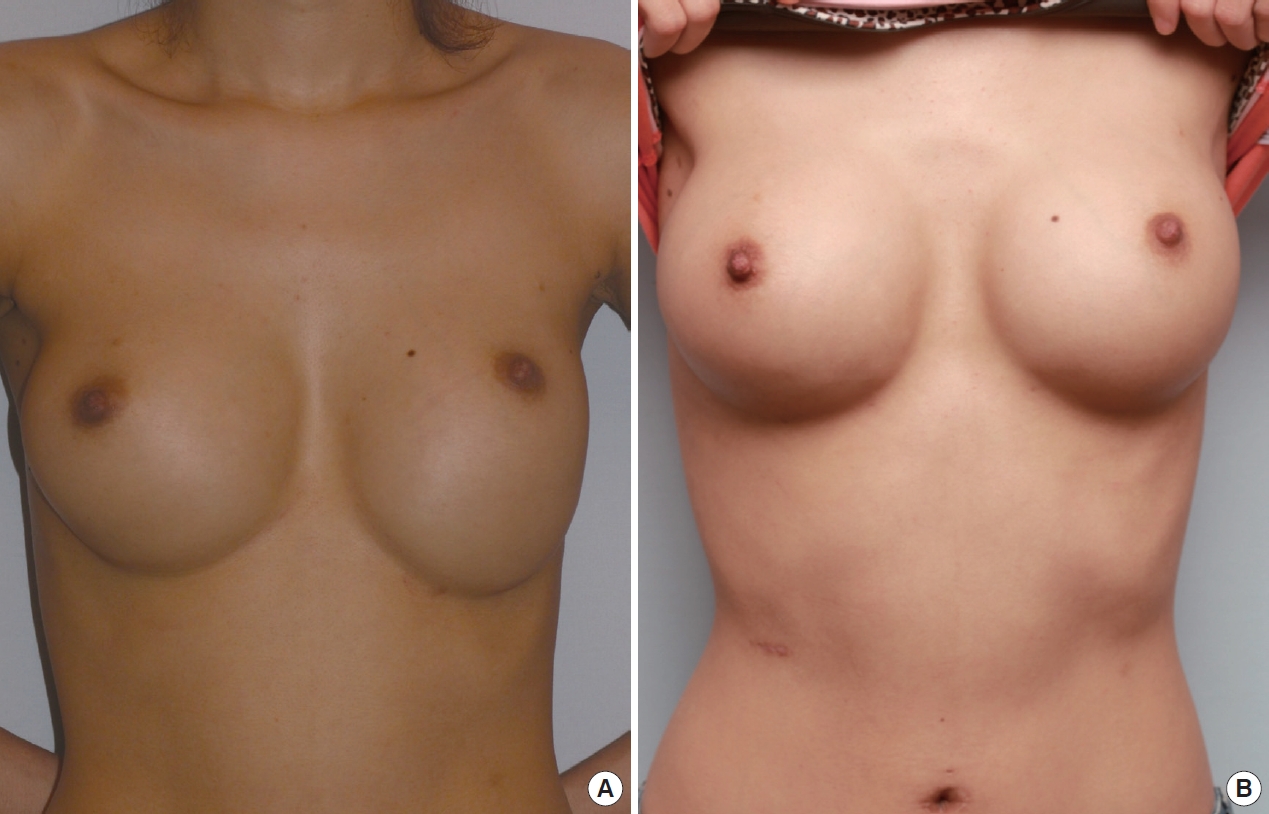
An incision was made on the axilla, 4 cm in length, with a #15 blade and deepened with a Bovie electrocoagulator. Upon approaching the upper capsule, capsulotomy was performed with the Bovie electrocoagulator using a breast endoscope (Richard-Wolff, Knittlingen, Germany). The previous implant was removed and a new inframammary fold was created by electrocauterization, causing lower pole contraction with an electrocoagulator. The power of the electrocoagulator (Megapower, Megadyne, Draper City, UT) was set to 45 W during the procedure. Electrocauterization was performed 1 cm above the new inframammary fold, because inferior migration of the implant was anticipated, although a textured surface implant was integrated into the breast tissue (Fig. 1). A Sebbin SM 325 cc (Sebbin, Pontoise, France) anatomically textured implant was inserted. Postoperatively, a brassiere was worn by the patient and there was no sign of recurrence during the 3-month follow up (Fig. 2).
Case 2
A 26-year-old patient visited our clinic after breast augmentation with a silicone implant. During the initial surgery, smooth, round, cohesive implants (250 cc) were inserted into both subpectoral planes using a subareolar approach. We also used endoscopy to correct bottoming out via an axillary approach; only scar revision was performed at the previous subareolar incision site. Surgical procedures were similar with previous cases. Allergan 410MF 330 cc anatomically textured implants were inserted. The inferiorly displaced implant was maintained in a more upward position for 3 months after the procedure (Fig. 3).
DISCUSSION
Compared to conventional open surgery, endoscopy has advantages, such as smaller scars, less postoperative pain, and shorter hospitalization times. Due to its merits and successful usage in general surgery, interest in endoscopy in the field of plastic surgery has grown since the early 1990s. Currently, forehead/brow lifts, transaxillary breast augmentation, and abdominoplasty are the most commonly practiced endoscopic plastic surgeries [10]. Especially during breast surgery, transaxillary breast augmentation, breast reconstruction with a latissimus dorsi flap, capsulotomy, capsulectomy, capsulorrhaphy, lowering or resuspension of the inframammary fold, and implant exchange are performed with an endoscopic approach.
Bottoming out occurs from the inferior malpositioning of the breast implant after breast augmentation; several factors contribute to the condition: Quality of the breast envelope, especially thickness of the subcutaneous tissue, and quality of the dermis, which is prone to lower pole expansion are important contributors. Smooth implants tend to cause bottoming out more frequently than do textured implants, since textured implants adhere to the breast capsule that results in stability, whereas smooth implants are not prone to adhesion. In addition, the particular approach for breast augmentation is an important factor. Unlike transaxillary and inframammary fold approaches, transumbilical breast augmentation has been correlated to bottoming out [11], since it involves dissection of the lower pole, especially the inframammary folds.
In the second case, we used an axillary approach, although the previous breast augmentation surgery was performed via a periareolar approach. Correction of bottoming out can be performed at the previous incision site, but significantly increased rates of capsular contracture have been reported with the use of periareolar approaches in some previous studies [12-14]. Therefore, the authors conducted only scar revision of the widened periareolar scar, whereas the correction of bottoming out was performed using an additional axillary incision.
Conventional techniques for correcting implant inferior malposition involve capsulectomy and capsulorrhaphy via inframammary fold incisions, which are prone to cause large scars. However, in this report, we present a novel technique for bottoming out correction using an endoscopic approach that is not only simple but also leaves a smaller scar. With only an axillary incision, bottoming out can be corrected by electrocauterization of the capsule, which easily causes lower pole contraction.
However, there are limitations to the procedure, owing to the endoscopic approach itself. While small incisions enable small scars and a shorter recovery period, they also limit the range of motion and surgical field. Hence, in cases of severe malpositioning, endoscopy is not recommended since correct positioning cannot be accomplished compared to open surgery. Since this procedure is performed just at the capsule surrounding the implant, there may be a low possibility of thermal injury to the skin envelope.
Another limit of this study is the relatively short follow-up period. The authors describe a small number of patients who underwent electrocauterization to correct bottoming out; all patients in this report visited our clinic 3 months after surgery. Long-term observation is necessary to elucidate the definitive effects of this procedure, because recurrence of bottoming out can occur after 3 months.
However, bottoming out is usually associated with implant surgery using a transumbilical approach with saline-filled implants. When textured implants are used, there is tissue integration of the implant with the normal tissue, which assumes minimal migration unless complications, such as a double-capsule deformity, occur.
In conclusion, we present a novel technique that is simple and effective for managing inferior implant malposition, ŌĆśbottoming out,ŌĆÖ using endoscopy-assisted electrocauterization. Due to its short surgical time, endoscopy was able to result in a high level of satisfaction among the ŌĆśbottoming outŌĆÖ patients.