 |
 |
- Search
| Arch Aesthetic Plast Surg > Volume 24(1); 2018 > Article |
|
Abstract
Background
The donor site of abdominal flaps for breast reconstruction consists of a wide suprafascial cavity that poses a risk of seroma formation. The authors evaluated the efficacy of continuous progressive tension sutures (PTS) using unidirectional barbed absorbable sutures for decreasing the volume of fluid collection and the risk of seroma at the abdominal donor site.
Methods
Between March 2013 and February 2015, 37 consecutive patients underwent breast reconstruction using a deep inferior epigastric artery perforator flap. Two patients who underwent salvage operations were excluded. Ten patients underwent standard abdominal flap donor site closure without PTS. Seven received donor site closure with interrupted Vicryl PTS between the abdominal flap and abdominal muscle fascia. Eighteen patients underwent closure with continuous PTS using unilateral barbed absorbable sutures. Body mass index, the approximate flap area, the duration of drain maintenance, the total drained volume, and the incidence of seroma were compared across these 3 groups. The operative time and subjective difficulty perceived by the surgeon was compared between the 2 PTS groups.
Results
The total drained volume was lower and the duration of drain maintenance was shorter in both PTS groups than in the standard closure group. There were no cases of seroma in the PTS groups, and 2 that resolved with conservative care in the standard closure group. More time was required and the subjective difficulty score was significantly higher for interrupted PTS than for continuous PTS.
Breast reconstruction using abdominally based free flaps has steadily become more popular, becoming the first-line choice for autologous breast reconstruction. Since Hartrampf et al. [1] introduced the pedicled flap to transfer superior epigastric artery-based tissue with the rectus abdominis muscle as a carrier, abdominal musculocutaneous or fasciocutaneous tissue has been a major component of breast reconstruction. Abdominally based flaps have the major advantage of providing ample volume with tissue supplied by a reliable pedicle, while simultaneously redefining the contour of the abdomen. However, a disadvantage of the technique is the potential for donor site morbidity, including muscle diastasis, abdominal wall bulging, and hernia [2]. The incidence of such problems has significantly decreased since the introduction of muscle-sparing methods of flap elevation, including muscle-sparing transverse rectus abdominis (TRAM) flaps, superficial inferior epigastric artery perforator (SIEA) flaps, and deep inferior epigastric artery perforator (DIEP) flaps [2-5].
However, even such muscle-sparing abdominal flaps produce a wide suprafascial cavity in the abdominal area that poses the risk of seroma formation [6]. A 10-year review by Gill et al. [7] of 758 patients who underwent DIEP flap breast reconstruction found a 5% incidence of donor site seroma and a 0.7% incidence of abdominal hernia. While seroma is not considered to be a severe complication, its management is labor-intensive for the patient, usually involving multiple visits in a short time frame to an outpatient clinic for drainage with or without compressive dressing. Left untreated, the seroma can lead to the formation of a surrounding capsule that may require surgical removal.
Many reports have studied the efficacy of drains, fibrin sealants, quilting sutures, and progressive tension sutures (PTS) for reducing seroma incidence at musculocutaneous flap donor sites [8-11]. Quilting sutures (stitches between the subcutaneous tissue of the elevated flap and the underlying abdominal muscle aponeurosis or fascia) have been found to show significant protective effects in reducing seroma at the donor sites of TRAM flaps, abdominoplasty regions, and latissimus dorsi muscle flaps [12,13]. While almost all reports differ in terms of the suture material, suture location, and number of stitches, the standard procedure involves using size 0 to #2-0 absorbable or nonabsorbable filaments to fix the abdominal flap down to the fascia with interrupted sutures [12,13]. The major downside of this procedure is that it requires additional operative time.
The authors, by using barbed absorbable sutures in a continuous running method, aimed to reduce the additional time and energy that this technique requires. Barbed sutures, developed by the plastic surgeon Gregory Ruff, have been applied in many settings in plastic surgery, including facelifts and skin closure [14,15]. The main advantage of this material is the elimination of the knotting process required for interrupted sutures; this innovation reduces the operative time and distributes the wound tension across multiple barbs rather than the knotted end.
This study was conducted to evaluate the efficacy of continuous barbed absorbable sutures, compared with conventional absorbable interrupted sutures, for closing abdominal DIEP flap donor sites.
This study was approved by the Institutional Review Board of the Catholic University of Korea (KC15RISI0383). The study was performed in accordance with the ethical standards of the 1964 Declaration of Helsinki and subsequent amendments.
All patients who underwent DIEP flap reconstruction for unilateral breast cancer between March 2013 and February 2015 at Seoul St. Mary’s Hospital were included. The patient’s age, body mass index (BMI), history of previous abdominal surgery, and smoking history were noted. The exclusion criteria were patients who underwent any additional salvage operations in the first week after reconstruction, smokers, and those with uncontrolled diabetes mellitus or autoimmune diseases.
All patients were operated on by the same surgical team. The periumbilical flap design was made preoperatively, and the flap size was adjusted according to the estimated area of mastectomy skin resection. After mastectomy, breast reconstruction was performed using a DIEP flap. The dimensions of the flap were determined based on the estimated area of skin resection. The approximate flap area was calculated as follows: (maximal width of the flap [cm])×(maximal length of the flap [cm]).
The caudal and cranial abdominal flaps were raised along the suprafascial layer using monopolar electrocautery (Bovie Medical, Clearwater, FL, USA) at a power setting of 25 to 40 W for both the cutting and coagulation modes. The cranial limit was the xiphoid process and the costal borders, and the caudal limit was the inguinal ligaments laterally, and 2 cm above the symphysis pubis at the midline. After the operating table was adjusted to the Fowler position (head of the bed raised 30° and hips semi-flexed), the cranial and caudal abdominal flaps were approximated using 3 different methods.
Conventional group: Before October 2013, the surgical team did not perform any quilting sutures at the abdominal donor sites. The cranial and caudal flaps were brought together by knotting the two flaps together with #1-0 Vicryl sutures between the Scarpa fascia.
The interrupted PTS group: From October 2013 to March 2014, 6–8 interrupted PTS were performed along the midline of the cranial abdominal flap, between the xiphoid process and the umbilical stalk. The sutures were applied while pulling the cranial flap in a caudal vector in order to decrease the tension burden upon the margin of the flap. The time between the first needle penetration to the last scissoring of the last suture was recorded. The surgeon was asked to verbally evaluate the difficulty of the procedure immediately afterwards. A numerical score of 0 (very easy) to 5 (very difficult) was used.
The continuous PTS group: From March 2014 to February 2015, the authors used a single #2-0 absorbable unilateral barbed suture (V-LOC™ 90; Covidien, New Haven, CT, USA) to perform continuous PTS along the midline between the xiphoid process and umbilical stalk, making 6 to 8 loops between the flap and fascia (Fig. 1). The duration and subjective difficulty of the procedures were recorded as well.
In all 3 groups, umbilical transposition was performed, and fibrin sealant was sprayed along the walls of the cavity. Two 200-mL negative suction drains (Barovac SS200JP, 4.8 mm tube diameter; Sewoon Medical, Cheonan, Korea) were placed on the right and left sides of the abdominal cavity in every patient. The abdominal flaps were completely closed using #3-0 Vicryl sutures for the subcutaneous layer and #4-0 polydioxane sutures for the subcuticular layer. Surgical tape (Steri-Strips; Health Care, St. Paul, MN, USA) was applied for skin closure. An external compressive garment was wrapped around the abdomen.
The length of the PTS procedure was measured by calculating the time interval between the initiation of the first suture and the finalization of the last knot of the last suture. The surgeon was asked to verbally rate the difficulty of the procedure on a scale of 1 (very easy) to 5 (very difficult) immediately after the procedure.
All patients were instructed to maintain their hips in the flexed position (the Fowler position) during the immediate postoperative period. They wore an elastic garment that provided light compression. Early ambulation was encouraged, starting 24 hours after returning to the ward. Low-dose aspirin (100 mg/day) was administered for 1 week beginning on the day of the operation. The abdominal drains were removed when the total volume of fluid collected through a single drain during the previous 24 hours was less than 20 mL. The drain output was checked every 8 hours by the same nursing team. Drain function was checked twice every day and syringe aspiration of the drain was performed when blockage was suspected. The aspirated volumes were noted and added to the total drained volume.
The patient’s abdomen was observed once to twice daily by the surgical team and examined for any fluid accumulation or bulging of the abdomen. The length of hospital stay was around 1 week for all patients, and was extended when necessary (due to a delay in drain removal, flap or donor complications, or the patient’s request). Outpatient follow-up was conducted at 2 weeks, 1 month, 2 months, and 6 months after the operation.
Age, BMI, approximate flap area (defined as [maximal width of the flap]×[maximal length of the flap]), the total drain output volume, and the duration of drain insertion were compared across the 3 groups using analysis of variance and post hoc tests with the Bonferroni correction. The incidence of seroma was compared using the χ2 test. The operative time across groups was compared using the Mann-Whitney test. All tests were performed using SPSS version 20.0 (IBM Corp., Armonk, NY, USA). All statistical tests were performed at a significance level of 5% (P<0.05).
A total of 35 women in whom a mastectomy was performed for unilateral breast cancer were included. Reconstruction was performed by the same plastic surgery team using DIEP flaps. Ten patients underwent standard abdominal flap donor site closure without PTS. Seven received donor site closure with interrupted PTS between the abdominal flap and abdominal muscle fascia using absorbable Vicryl sutures. Eighteen patients underwent closure with continuous PTS using unilateral barbed absorbable sutures. The mean age of the patients was 47.02 years (range, 35–62 years). The mean age was 46.7 years in the group without PTS, 45.8 years in the interrupted PTS group, and 47.2 years in the continuous PTS group (Table 1). The mean BMI was 23.2 kg/m2 in the group without PTS, 22.39 kg/m2 in the interrupted PTS group, and 22.76 kg/m2 in the continuous PTS group. The mean approximate flap area was 528.3 cm2 in the group without PTS, 575.5 cm2 in the interrupted PTS group, and 512.1 cm2 in the continuous PTS group. None of the patients were current or previous smokers (Table 2). A total of 10 patients had undergone previous operations in the abdominal area, including cesarean sections, myomectomies, and laparoscopic cholecystectomies (Table 1). None had experienced operative procedures in which the area of the adipocutaneous flap was extensively manipulated.
All 3 groups were homogenous in terms of age (P=1.000), BMI (P=1.000), and approximate flap area (P=1.000).
The average volume of total abdominal site drainage was significantly lower in the interrupted PTS group (292.3 mL, P=0.020) and in the continuous PTS group (356.4 mL, P=0.030) than in the group without PTS (556.4 mL). No significant difference was found between the 2 PTS groups.
The duration of drain maintenance was significantly shorter in the continuous PTS group (5.69 days, P=0.016) than in the group without PTS (7.1 days). Drains were also removed earlier in the interrupted PTS group (5.71 days, P=0.139), but the difference was not statistically significant (Table 2).
The mean length of the hospital stay was 9.7 days in the group without PTS, 9.28 days in the interrupted PTS group, and 9.38 days in the continuous PTS group. These differences were not statistically significant.
Two patients in the standard closure group without PTS presented with a fluctuation in the abdominal area at the first outpatient visit at 2 weeks after the operation, and were treated with consecutive aspirations and compression garments. No cases of seroma took place in either PTS group (P=0.022).
The subjective difficulty score assigned by the surgeon immediately after the procedure was significantly lower (P<0.0001) in the continuous PTS group (1.27) than in the interrupted PTS group (3.42). The time it took for the surgeons to perform the procedure was also significantly shorter (P<0.0001) in the continuous PTS group (340 seconds) than in the interrupted PTS group (755.7 seconds).
Breast reconstruction using an abdominally based free flap has become the mainstream method of autologous breast reconstruction. Since Hartrampf et al. [1] introduced the pedicled rectus abdominis muscle flap, abdominally based flaps have continuously been refined in order to provide a large volume of well-vascularized tissue, while simultaneously minimizing donor site complications. The development of the DIEP and SIEA flaps has focused on donor site protection. The incidence of major complications, including muscle diastasis, abdominal wall bulging, and abdominal hernia has decreased with the development of methods that spare the rectus abdominis muscle and/or fascia [2]. A notable and significant difference is present in this regard between patients who undergo bilateral TRAM reconstruction and those who undergo bilateral DIEP or SIEA reconstructions.
Seroma formation is a relatively common donor site complication that occurs after abdominal flap breast reconstruction. Its reported incidence ranges from 2% to 10% [16]. Seroma formation is a nuisance for the patient, a factor that decreases satisfaction, and requires additional visits to an outpatient clinic or to the operating room when surgical intervention is necessary.
While the exact etiology of seroma remains unknown, several hypotheses have been suggested. Some considered the fluid to be lymphorrhea from damaged lymphatic vessels, and surgeons reported that preserving the Scarpa fascia during elevation of the abdominal flap in lipoabdominoplasty patients decreased seroma formation, because of the lower incidence of blood vessel injuries and because the Scarpa fascia was considered to be a structure that played a major role in absorbing lymphatic fluid [17,18]. Andrades and Prado [19] analyzed seroma fluid, finding that it resembled inflammatory exudate more closely than it resembled lymphatic fluid, as indicated by higher levels of total proteins, lactate dehydrogenase, cholesterol, and neutrophils. They speculated that thermal damage caused by electrocautery resulted in seroma formation, and reported that clinical studies comparing scalpel dissection versus electrical dissection corroborated this laboratory-based hypothesis. McCarthy et al. [20] suggested that the presence of dead space and friction between the 2 tissue interfaces may potentiate seroma formation.
The known predisposing factors for seroma formation at the abdominal donor site are high BMI, the use of SIEA flaps instead of DIEP or TRAM flaps, and bilateral reconstruction [21-24]. Electrocautery and thermal injury are also factors that have recently received attention in this regard [17,19]. It is reasonable to speculate that the larger the area of dissection, the more thermal or physical injury occurs to the vasculature or lymphatics, making seroma formation more likely. Considering the emerging evidence that obesity is a risk factor for both premenopausal and postmenopausal breast cancer, surgeons should be prepared with the right tools to overcome the complications, including seroma, that accompany reconstruction in high-BMI patients [25].
Many technical modifications and advances have been suggested in the search to prevent seroma formation. Methods of dissection include refraining from electrocautery, minimizing the area of dissection, and preserving the Scarpa fascia. Additive procedures during closure aim to accelerate the elimination of the subcutaneous dead space. Fibrin sealant or glue, quilting sutures, or PTS applied to the musculocutaneous flap donor site or abdominoplasty flap have all been shown to be effective by various authors [8-11]. Quilting sutures using the progressive tension method have been found to exert significant protective effects in terms of reducing seroma at the donor sites of TRAM flaps, abdominoplasty regions, and latissimus dorsi muscle flaps [12,13]. While almost all reports differ in terms of the suture material, suture location, and number of stitches, the standard procedure involves using size 0 to #2-0 absorbable or nonabsorbable filaments to fix the abdominal flap down to the fascia with interrupted sutures [12,13].
With the introduction of barbed absorbable sutures, developed by the plastic surgeon Gregory Ruff, surgeons became able to skip the knotting process and to apply sutures efficiently in various procedures. Beginning with facelifts and skin closure, many groups have used this material during abdominal flap closure [14,15]. Nagarkar et al. [26] found that the application of running barbed PTS along the entire elevated flap, combined with limited dissection, allowed the surgeon to even obviate the requirement for drain placement at the donor site. The main advantage of this material is the elimination of the knotting process required for interrupted sutures; this innovation reduces the operative time and distributes the wound tension across multiple barbs rather than the knotted end. Pollock and Pollock found that PTS transferred the tension of the flap to the fascial system, enabling the surgeon to perform skin closure under minimal tension.
The authors applied barbed PTS to the supraumbilical midline of the abdominal flap, along the linea alba. This anatomical structure is where the abdominal flap adheres to the aponeuroses of the abdominal muscles, meaning that sutures placed here will not cause abnormal adhesion or dimpling. The authors found that the total drained volume was lower and the duration of drain maintenance was shorter in both PTS groups than in the standard closure group. It is worth emphasizing that all groups were homogeneous in terms of age, BMI, and elevated flap area.
There were no cases of seroma in the PTS groups, and 2 cases that resolved with conservative care in the standard closure group. The only disadvantage of the continuous PTS group was the additional cost of the unilateral barbed sutures. However, a single V-LOC suture (V-LOC™ 90; Covidien) was required for the length of PTS in each patient, from the xiphoid process to the umbilicus, so the additional cost burden (in the case of our hospital) was around 29 United States Dollar. Considering the conservation of operative time and surgeon energy, the comprehensive benefits of the continuous PTS method make it superior to the conventional PTS method.
Unlike other studies, there was no significant difference in the duration of hospital stay, which was probably due to the fact that patients were not discharged based on removal of their donor site drains, but under the influence of a variety of factors, including private insurance, subjective discomfort, and caretaker availability.
Although Nagarkar et al. [26] showed that increasing the number of continuous barbed PTS in the abdominal area may contribute to the elimination of donor site drains, we believe that several factors should be evaluated first. The effectiveness of the additional cost and operative time should be considered, as well as the possible cosmetic effects of the quilting material integrated along the entire abdomen. Further prospective studies are warranted to evaluate the point of maximum efficiency [15,16].
Fig. 1.
A drawing of the sagittal section of the abdomen during closure. The barbed sutures passed through the Scarpa fascia and the abdominal fascia in a caudal direction.
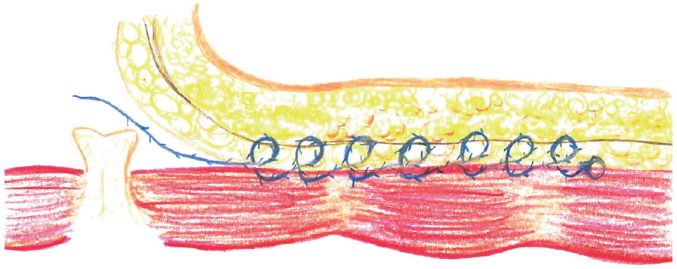
Table 1.
Patient demographics
Table 2.
Surgical data of the 3 groups
| Group | Standard closure | Interrupted PTS | P-value | Continuous PTS | P-value |
|---|---|---|---|---|---|
| No. of patients | 10 (28.6%) | 7 (20.0%) | 18 (51.4%) | ||
| Donor flap area (cm2) | 528.3 ± 72.8 | 575.5 ± 120.6 | 1.000 | 512.1 ± 88.4 | 1.000 |
| Body mass index (kg/m2) | 23.2 ± 1.60 | 22.39 ± 2.20 | 1.000 | 22.76 ± 2.84 | 1.000 |
| Total drained volume (mL) | 556.4 ± 239.0 | 292.3 ± 112.3 | 0.020 | 356.4 ± 172.9 | 0.030 |
| Drain removal day (postoperative day) | 7.1 ± 1.44 | 5.71 ± 0.63 | 0.139 | 5.69 ± 1.32 | 0.016 |
| No. of patients with seroma | 2 (5.7%) | 0 (0.0%) | 0 (0.0%) | ||
| Duration of PTS procedure (s), mean | 756 | 340 | |||
| Subjective difficulty of PTS (scale)a) | 3.42 | 1.27 | <0.0001 |
REFERENCES
1. Hartrampf CR, Scheflan M, Black PW. Breast reconstruction with a transverse abdominal island flap. Plast Reconstr Surg 1982;69:216-25.


2. Blondeel N, Vanderstraeten GG, Monstrey SJ, et al. The donor site morbidity of free DIEP flaps and free TRAM flaps for breast reconstruction. Br J Plast Surg 1997;50:322-30.


3. Salgarello M, Tambasco D, Farallo E. DIEP flap donor site versus elective abdominoplasty short-term complication rates: a meta-analysis. Aesthetic Plast Surg 2012;36:363-9.


4. Kim BJ, Choi JH, Kim TH, et al. The superficial inferior epigastric artery flap and its relevant vascular anatomy in Korean women. Arch Plast Surg 2014;41:702-8.



5. Holm C, Mayr M, Hofter E, et al. The versatility of the SIEA flap: a clinical assessment of the vascular territory of the superficial epigastric inferior artery. J Plast Reconstr Aesthet Surg 2007;60:946-51.


6. Sadeghi A, Malata C. Persistent seromas in abdominal free flap donor sites after postmastectomy breast reconstruction surgery: case reports and literature review. Eplasty 2013;13:e24.


7. Gill PS, Hunt JP, Guerra AB, et al. A 10-year retrospective review of 758 DIEP flaps for breast reconstruction. Plast Reconstr Surg 2004;113:1153-60.


9. Nahas FX, di Martino M, Ferreira LM. Fibrin glue as a substitute for quilting suture in abdominoplasty. Plast Reconstr Surg 2012;129:212e-3e.


10. Pollock T, Pollock H. Progressive tension sutures in abdominoplasty. Clin Plast Surg 2004;31:583. -9. vi.


11. Pollock TA, Pollock H. Progressive tension sutures in abdominoplasty: a review of 597 consecutive cases. Aesthet Surg J 2012;32:729-42.



12. Lee KT, Mun GH. Fibrin sealants and quilting suture for prevention of seroma formation following latissimus dorsi muscle harvest: a systematic review and meta-analysis. Aesthetic Plast Surg 2015;39:399-409.


13. Rossetto LA, Garcia EB, Abla LE, et al. Seroma and quilting suture at the donor site of the TRAM flap in breast reconstruction: a prospective randomized double-blind clinical trial. Ann Plast Surg 2014;72:391-7.


14. Rosen AD. New and emerging uses of barbed suture technology in plastic surgery. Aesthet Surg J 2013;33:90s. 5s.


16. Nahabedian MY. Secondary operations of the anterior abdominal wall following microvascular breast reconstruction with the TRAM and DIEP flaps. Plast Reconstr Surg 2007;120:365-72.


17. Sowa Y, Numajiri T, Kawarazaki A, et al. Preventive effects on seroma formation with use of the harmonic focus shears after breast reconstruction with the latissimus dorsi flap. J Plast Surg Hand Surg 2016;50:349-53.


18. Saldanha OR, Federico R, Daher PF, et al. Lipoabdominoplasty. Plast Reconstr Surg 2009;124:934-42.


19. Andrades P, Prado A. Composition of postabdominoplasty seroma. Aesthetic Plast Surg 2007;31:514-8.



20. McCarthy C, Lennox P, Germann E, et al. Use of abdominal quilting sutures for seroma prevention in TRAM flap reconstruction: a prospective, controlled trial. Ann Plast Surg 2005;54:361-4.


21. Moradi P, Durrant C, Glass GE, et al. SIEA flap leads to an increase in abdominal seroma rates compared to DIEP flap for breast reconstruction. Eur J Plast Surg 2011;34:87-91.

22. Momeni A, Ahdoot MA, Kim RY, et al. Should we continue to consider obesity a relative contraindication for autologous microsurgical breast reconstruction? J Plast Reconstr Aesthet Surg 2012;65:420-5.


23. Wu LC, Iteld L, Song DH. Supercharging the transverse rectus abdominis musculocutaneous flap: breast reconstruction for the overweight and obese population. Ann Plast Surg 2008;60:609-13.


24. Gabbay JS, Eby JB, Kulber DA. The midabdominal TRAM flap for breast reconstruction in morbidly obese patients. Plast Reconstr Surg 2005;115:764-70.








