|
 |
- Search
| Arch Aesthetic Plast Surg > Volume 28(3); 2022 > Article |
|
Abstract
Spontaneous inflation of saline breast implants is a rare phenomenon. In this case report, we share our experience treating a patient who complained of asymmetric breasts from what appeared to be a straightforward case of capsular contracture. Spontaneous autoinflation of the right breast implant was subsequently found to be the cause of breast asymmetry and hardness. The presentation, diagnostic challenge, management, and mechanism of this rare phenomenon are presented here.
Controversy over the safety of silicone gel-filled implants led to the temporary popularity of saline-filled implants in the 1990s. During that time, saline-filled mammary implants had lower complication rates than silicone breast implants, which had presented with complications such as capsular contracture, rupture, gel bleed, and migration [1]. The most common complication unique to saline implants was deflation [2]. Although saline breast implants are outdated in current practice, the long-term complications can still be seen, as in this case.
We report a case of autoinflation, an unusual complication in a saline implant, which was initially thought to be a straightforward case of capsular contracture because of their similar properties (i.e., hardening, pain, and spherical enlargement of the breast).
A 58-year-old patient presented to our institution complaining of gradual breast hardening and asymmetry. She had received bilateral breast augmentation with permanent implants 15 years earlier. She did not recall the type or model of the implants.
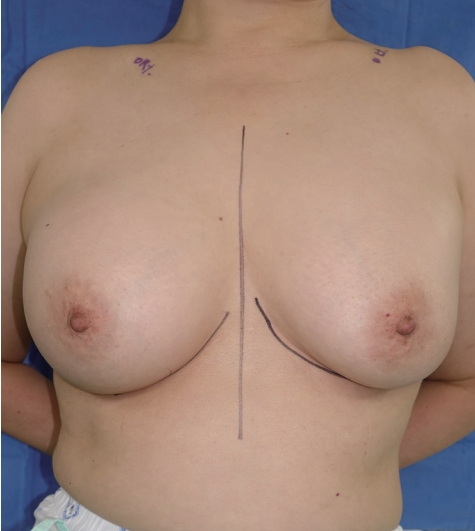
On physical examination, the right breast was harder than the left breast, and upper pole fullness was evident on the right breast when compared to the left breast. The patient complained of stretching pain on the right side. The right nipple-areolar complex was drawn cranially (Fig. 1). Mammography was nonspecific. The patient was taking medications to control diabetes mellitus, hypothyroidism, and dyslipidemia. With a preliminary diagnosis of right-sided capsular contracture, bilateral total capsulectomy and implant removal were planned.
Under general anesthesia, a bilateral inframammary crease incision was utilized. Contrary to our expectation, a thin layer of capsule was noted around the right implant. Total capsulectomy was possible on both sides without violation of the capsule or rupture of the implants. After unviolated total capsulectomy, the remnant right breast pocket was intact without signs of infection or fibrosis. However, as a precautionary measure, the explanted breast pockets were thoroughly irrigated with triple-antibiotic solution and closed in the usual fashion with negative suction drains. The patient preferred not to have new implants after explantation.
After removal of the implants, it was confirmed that both left and right implants were of the same model and volume (190 cc, textured, saline filled). However, the implant on the right was significantly larger and spherical in shape rather than the normal dome shape (Fig. 2). Despite the volume difference, the hyperinflated implant was grossly intact. The valve mechanism at the base of the implant was undisturbed. Based on these findings, autoinflation of the right-side implant was suspected.
The internal fluid from both implants was evacuated. The total aspiration volume of the autoinflated implant was 275 cc, compared to 180 cc in the contralateral implant, corresponding to a 40% inflation from the native volume. The gross appearance of the fluid was also different. The aspirate from the autoinflated implant showed a yellowish discoloration (Fig. 2C).
Chemical analysis of the aspirated fluids from both the normal and the autoinflated implants was performed (Table 1). Compared to the aspirate from the left implant, a significantly higher concentration of total protein was noted in the right. The albumin concentration was also nine times higher. Moderate amounts of red and white blood cells were also found.
Autoinflation of breast implants is a rare phenomenon that has been documented only in saline-filled breast implants. In the early 1990s, the safety of silicone-filled implants was questioned and saline implants gained popularity. Saline implants were considered less toxic, with a lower incidence of capsular contracture, as well as a lower rate of gel bleeding and migration [3]. Silicone-filled implants later regained popularity with the advent of a newer generation of silicone elastomers. Saline-filled implants are seldom used today, but their long-term consequences can still be seen. In contrast to the dramatic and widely recognized complication of sudden deflation, autoinflation of saline implants has received little attention in the literature [4].
Botti and Villedieu [5] first reported breast implant autoinflation, describing the abnormal enlargement of a double-lumen saline breast implant. They attributed this phenomenon to a dysfunctional outer valve, which might have acted as a unidirectional check valve to prevent the efflux of body fluid from the implant once it had migrated inside. Only anecdotal case series and reports followed, with insufficient information to determine the exact mechanism of this complication. Our PubMed search for ŌĆ£saline breast implant autoinflationŌĆØ yielded nine results, including five studies that presented clinical findings (Table 2). Most articles reported discolored, turbid fluid accumulation in the autoinflated implant with high osmolarity and protein content. Most cases also occurred unilaterally. Bilateral autoinflation was only found in one case, but detailed findings were not provided [5].
The mechanism of implant autoinflation has not been clearly elucidated. However, there are two hypotheses for the phenomenon. The most straightforward hypothesis suggests that a defect in the valve integrity is responsible for autoinflation. The faulty inflation valve, which is designed to permanently seal off after the initial instillation of the normal saline, becomes leaky and might act as a check valve [5]. Another hypothesis, termed the ŌĆ£osmotic swellingŌĆØ theory, proposes that the silicone elastomer shell is a semipermeable membrane that permits an osmotic fluid shift, leading to swelling of the implant without disruption of the implantŌĆÖs integrity [4]. In the early 2000s, the osmotic swelling theory fell out of favor due to research by Walter and Wolfram, who analyzed the fluid inside the autoinflated implant using biochemical analysis methods [6]. Their analysis identified glucose and protein in the implant fluid, both of which have high molecular weights and cannot pass through the implant shell by osmotic shift [7]. Furthermore, protein analysis with gel electrophoresis showed that the spot pattern of the implant fluid was very similar to the patientsŌĆÖ serum, indirectly proving the origin of the additional fluid volume [3]. In line with these studies, our case also identified high amounts of protein, which supports the faulty valve theory.
A peculiar feature of our case is the time to diagnosis of autoinflation after augmentation. A literature search showed that time to patient presentation ranged from 6 to 120 months (Table 2). Our patient presented to the clinic after 15 years, which is the longest interval before patient presentation in the reported literature. The reason for this delay in presentation is not clear, but the patientŌĆÖs wide body habitus and greater skin thickness may have played a role in the delayed recognition of the unilateral autoinflation.
It should be pointed out that autoinflated implants can mimic high-grade capsular contracture in terms of upward migration, spherical deformation, stiffness, and pain. The impression of autoinflation is further confounded because most patients do not recall the model or material properties of their implants. In our case, we were not able to obtain an implant-related history from the patient or from the previous hospital and therefore presumed that the patient had developed capsular contracture, a common and reasonable explanation for the patientŌĆÖs symptoms. Routine mammograms were not enough to evaluate the degree of capsular contracture. In retrospect, performing an ultrasound or magnetic resonance imaging examination might have differentiated autoinflation from capsular contracture. However, we did not feel it was necessary to perform a costly examination since the findings were very similar to high-grade capsular contracture, and the prosthesis was old enough to consider explantation. The medical history and physical examination provided more than sufficient findings to think that capsulectomy and implant removal were indicated for the patient.
Although seldom used in current practice, previously inserted saline implants require follow-up care. In this context, we think that the rare phenomenon of autoinflation in a saline implant is noteworthy.
Notes
Ethical approval
This study was approved by the Institutional Review Board of The Catholic University of Korea College of Medicine (IRB No. KC22- ZASI0221).
Patient consent
The patient provided written informed consent for publication of the case and the use of her images.
Fig.┬Ā2.
Explanted implant, capsule, and aspirated fluid from inside the implant. (A) Total capsulectomy was performed without violating the implant integrity. Both implants were textured saline implants of the same volume. The capsulectomy specimen was nonspecific and did not show a high degree of contracture. (B) Although the two implants were of the same model, overinflation is noted in one implant (on the left). (C) The color and turbidity of the aspirate are deeper yellow and viscous (left syringe) compared to the normal aspirate (right syringe).

Table┬Ā1.
Chemical analysis of the fluid inside an autoinflated saline implant compared to an unaffected saline implant
| Measurement | Autoinflated side (right) | Normal side (left) |
|---|---|---|
| Total protein (┬Ąg/mL) | 1,119.5 | 1.8 |
| Albumin (g/dL) | 0.91 | <0.1 |
| pH | 7.6 | 7.2 |
| Color | Yellow | Colorless |
| Specific gravity (g/cm3) | 1.012 | 1.005 |
| White blood cell count (/┬ĄL) | 605a) | 1 |
| Red blood cell count (/┬ĄL) | 1,200 | 0 |
| Chloride (mEq/L) | 130 | 153 |
| Glucose (mg/dL) | <10 | <10 |
| Osmolality (mOsm/kg) | 299 | 293 |
| Lactate dehydrogenase (IU/L) | <50 | <50 |
Table┬Ā2.
Summary of previous literature reporting autoinflation of saline implants
| No. of subjects | Lumen | Texture | Interval to symptom occurrence (mo), range | Gross description of implant fluid | Increase of volume (%), range | Chemical analysis | Reference |
|---|---|---|---|---|---|---|---|
| 1 | Double | Textured | 6 | Brown colored, thick | NA | NA | [5] |
| 2 | Single | Textured | 8 | Brown colored, thick, or clear | 15 | Negative bacterial culture | [7] |
| 3 | NA | Smooth | 45-87 | Brown colored, thick | 45-87 | Hyperosmolar, high in sodium and chloride, positive bacterial culture | [2] |
| 3 | Single | Smooth | 86-108 | Highly viscous | 15-114 | High protein content, hyperosmolar | [6] |
| 1 | Single | Smooth | 120 | Dark yellow, more viscous | NA | Electrophoresis results similar to patientŌĆÖs serum | [3] |
REFERENCES
1. Robinson OG Jr, Benos DJ, Mazzochi C. Spontaneous autoinflation of saline mammary implants: further studies. Aesthet Surg J 2005;25:582-6.


2. Peters W. Autoinflation of saline-filled inflatable breast implants. Can J Plast Surg 2006;14:219-26.



3. Wolfram D, Backovic A, Kaindl R, et al. Spontaneous unilateral autoinflation of a saline-filled mammary implant. J Plast Reconstr Aesthet Surg 2008;61:342-5.


4. Tuncali D, Ozgur F. Spontaneous autoinflation of saline-filled mammary implants: postoperative volume determination by magnetic resonance imaging. Aesthetic Plast Surg 1999;23:437-42.



5. Botti G, Villedieu R. Postoperative self-expansion in augmentation mammaplasty. Plast Reconstr Surg 1994;93:1310.