 |
 |
- Search
| Arch Aesthetic Plast Surg > Volume 23(2); 2017 > Article |
|
Abstract
Gynecomastia refers to persistent enlargement of the breast in males caused by enlargement of the breast bud and surrounding stroma. It typically occurs in newborns, during early adolescence, and in late adulthood. There are several pathological causes. If no pathological cause is evident, gynecomastia is considered idiopathic. The reported prevalence of unilateral gynecomastia is approximately 35% to 45%, but most previous reports have focused on distinctive pathologic causes. As such, few previous reports of idiopathic unilateral gynecomastia during early adolescence have been published. Herein, we report a case of idiopathic unilateral gynecomastia in an adolescent male.
Gynecomastia refers to persistent enlargement of the breast in males caused by enlargement of the breast bud and the surrounding fibrous connective tissue [1]. Enlarged breasts are observed in 65% of adolescent males, but they mostly regress with time [2]. Pathologically, gynecomastia can be explained by an imbalance in male and female sex hormones. If estrogen, the female sex hormone, increases and/or androgen, the male sex hormone, decreases, estrogen can overcome the inhibitory effects of androgen to stimulate breast tissue growth. This results in the proliferation of breast ducts and fibroblastic stroma. When this stimulus continues, the ducts and fibroblastic stroma become fibrotic, and gynecomastia becomes well established and irreversible [3]. Herein, we report a case of idiopathic unilateral gynecomastia during early adolescence. After checking the patient’s hormonal status, we performed subcutaneous mastectomy using a transverse areolar incision. This report also documents the clinical, laboratory, and gross examination findings along with the histological features of the case.
A 16-year-old adolescent male presented with a complaint of discomfort due to a 5-year-history of an enlarged left breast. His symptoms started spontaneously at puberty. He had no history of hospitalization, medication including hormone therapy, or traumatic events involving the breast. He was not obese and showed the usual secondary sex characteristics of males except for the enlarged left breast. The left breast was moderately enlarged with no excess skin (Simon classification IIA). Palpation of the enlarged breast revealed firm glandular tissue. No bruising, discoloration, erythema, or signs of inflammation were observed on the overlying skin (Fig. 1). Ultrasonography of the breast was performed to evaluate the underlying tissue, revealing an approximately 1.3-cm area of breast glandular tissue in the left breast. Serum levels of sex hormones, including human chorionic gonadotropin, follicle-stimulating hormone, luteinizing hormone, testosterone, estradiol, progesterone, 17-hydroxyprogesterone, and prolactin, as well as those of thyroid hormones, including thyroid-stimulating hormone, free T4, and T3, were within the normal range. A subcutaneous mastectomy was performed under general anesthesia using a transverse areolar incision. A gross examination of the excised specimen revealed a lump of firm glandular tissue weighing 221 g and measuring 7.0×5.0× 4.0 cm. Microscopic findings confirmed that the lump consisted of glandular rather than fatty tissue (pseudogynecomastia) (Fig. 2). The dressings over the wound were changed daily until the drain was removed and the patient returned for stitch removal 10 days postoperatively. No recurrence occurred during 5 months of follow-up (Fig. 1).
There are several pathological causes of gynecomastia: a) lack of testosterone (due to the congenital absence of testes, Klinefelter syndrome [KS; XXY syndrome], viral orchitis, trauma, castration, or renal failure); b) increased estrogen levels (due to testicular tumors [Leydig cells], hermaphroditism tumor, obesity, malnourishment, liver disease, or hyperthyroidism); c) use of drugs in 20% of all cases in adult men (anabolic steroids, digoxin, gonadotropins, cimetidine, or methyldopa); d) gynecomastia of unclear cause (chronic illness, human immunodeficiency virus, refeeding after starvation, hemodialysis); and e) other idiopathic causes. There are well-established algorithms for evaluating the causes of gynecomastia using a hormonal workup (serum human chorionic gonadotropin, luteinizing hormone, thyroxine, estradiol, testosterone, and prolactin levels) and an imaging workup (testicular ultrasound, chest radiography, abdominal computed tomography, and adrenal computed tomography or magnetic resonance imaging). If all the evaluated data are normal, gynecomastia is considered idiopathic, which is the most common type [4].
Gynecomastia usually starts as a painless enlargement of the breasts. When it enlarges progressively, patients may develop pain. Pseudogynecomastia (fatty breasts), which is common in obese men, should be differentiated from true gynecomastia. True gynecomastia consists of firm glandular tissue underneath the periareolar area that is diffusely located, with a disc-like shape resembling the female breast. It is usually bilateral, but it can be unilateral, which is suggestive of malignancy in elderly patients [5]. The reported prevalence of unilateral gynecomastia is approximately 35% to 45%, but the incidence of idiopathic unilateral gynecomastia is unclear [3,6]. The incidence of breast cancer in males is <1% of the total cases of breast cancer. The mean age of male patients with breast cancer is 65 years. The risk of male breast cancer increases in patients with KS and those with a positive family history. The probable signs of malignancy are: 1) unilateral enlargement, 2) hard or irregular breast tissue, 3) rapid enlargement, 4) recent onset, 5) fixed mass, 6) nipple or skin abnormalities, 7) pain, 8) mass >5 cm, and 9) axillary lymphadenopathy [7].
Simon classified gynecomastia into 4 groups: grade I, small breast enlargement without excess skin; grade IIA, moderate breast enlargement without excess skin; grade IIB, moderate breast enlargement with excess skin; and grade III, large breast enlargement with excess skin. Our patient had a moderately enlarged breast with no excess skin, corresponding to grade IIA. The surgical treatment options for gynecomastia depend on the underlying nature of the breast enlargement. If there is only isolated subareolar bud development, liposuction using a small incision may be an attractive approach in terms of scar formation. If there is stromal hypertrophy, an en bloc excision of the fibrous tissue is performed with skin excision as needed. In cases with a pathological cause, medical management with agents such as gonadotrophic antagonists, antiestrogens, or anti-prolactins is essential [1,8].
Our patient was diagnosed with idiopathic unilateral gynecomastia. He had no history of hospitalization, medication including hormone therapy, or traumatic events involving the breast. He was not obese and otherwise showed the usual male secondary sex characteristics. All laboratory findings were normal. Some physicians may judge this condition as physiologic gynecomastia and underestimate its severity; however, there can be underlying pathologic causes of gynecomastia, and this condition can be physically embarrassing and psychologically distressing for the patient. Gynecomastia can resolve completely if the underlying cause is treated before the breast tissue becomes fibrotic. Thus, when plastic surgeons encounter patients with gynecomastia, especially those in early adolescence, a complete evaluation should be performed to identify its pathological causes, and active treatment should be initiated.
Fig. 1.
Preoperative and postoperative photographs. Preoperatively, the left breast was moderately enlarged with no excess skin (A). A postoperative photograph taken 10 days after the operation reveals a reduced left breast and a linear scar (B).

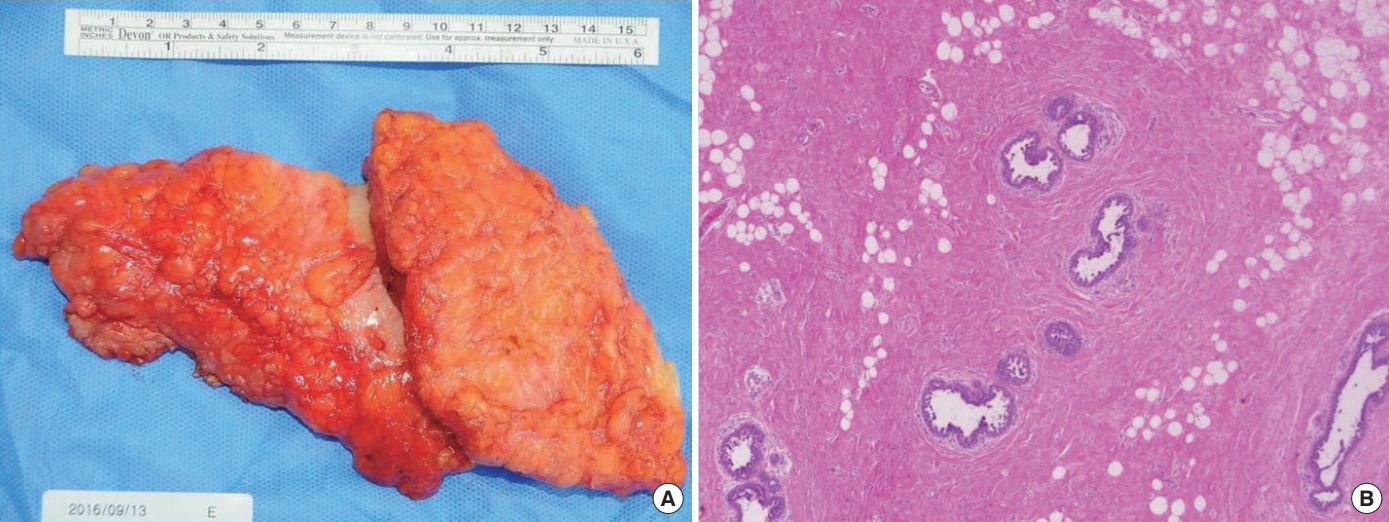
Fig. 2.
Gross examination of the excised specimen reveals a lump of firm glandular tissue weighing 221 g and measuring 7.0 × 5.0 × 4.0 cm (A). The ducts were surrounded by dense fibrous stroma and sparse adipose tissue without lobular tissue nodules (hematoxylin and eosin stain [H & E], original magnification ×40 magnification) (B).
REFERENCES
2. Lindsay RW, George R, Herberg ME, et al. Reliability of a standardized nasal anatomic worksheet and correlation with subjective nasal airway obstruction. JAMA Facial Plast Surg 2016;18:449-54.


3. Biro FM, Lucky AW, Huster GA, et al. Hormonal studies and physical maturation in adolescent gynecomastia. J Pediatr 1990;116:450-5.


6. Kumanov P, Deepinder F, Robeva R, et al. Relationship of adolescent gynecomastia with varicocele and somatometric parameters: a cross-sectional study in 6200 healthy boys. J Adolesc Health 2007;41:126-31.


-
METRICS

- Related articles in AAPS
-
Rapidly growing juvenile xanthogranuloma in an adult: a case report2023 January;29(1)





